Introduction
Understanding the complexities of HIPAA compliance is essential for any organization that handles protected health information (PHI). As regulations evolve and the risks associated with data breaches increase, organizations must navigate a landscape that requires not only adherence but also a proactive approach to compliance. This article explores best practices for effective HIPAA consultation, providing insights into how entities can strengthen their compliance programs, improve staff training, and implement rigorous monitoring and auditing processes.
How can organizations ensure they are not merely compliant but also prepared for the challenges posed by an ever-changing regulatory environment?
Understand HIPAA Compliance Fundamentals
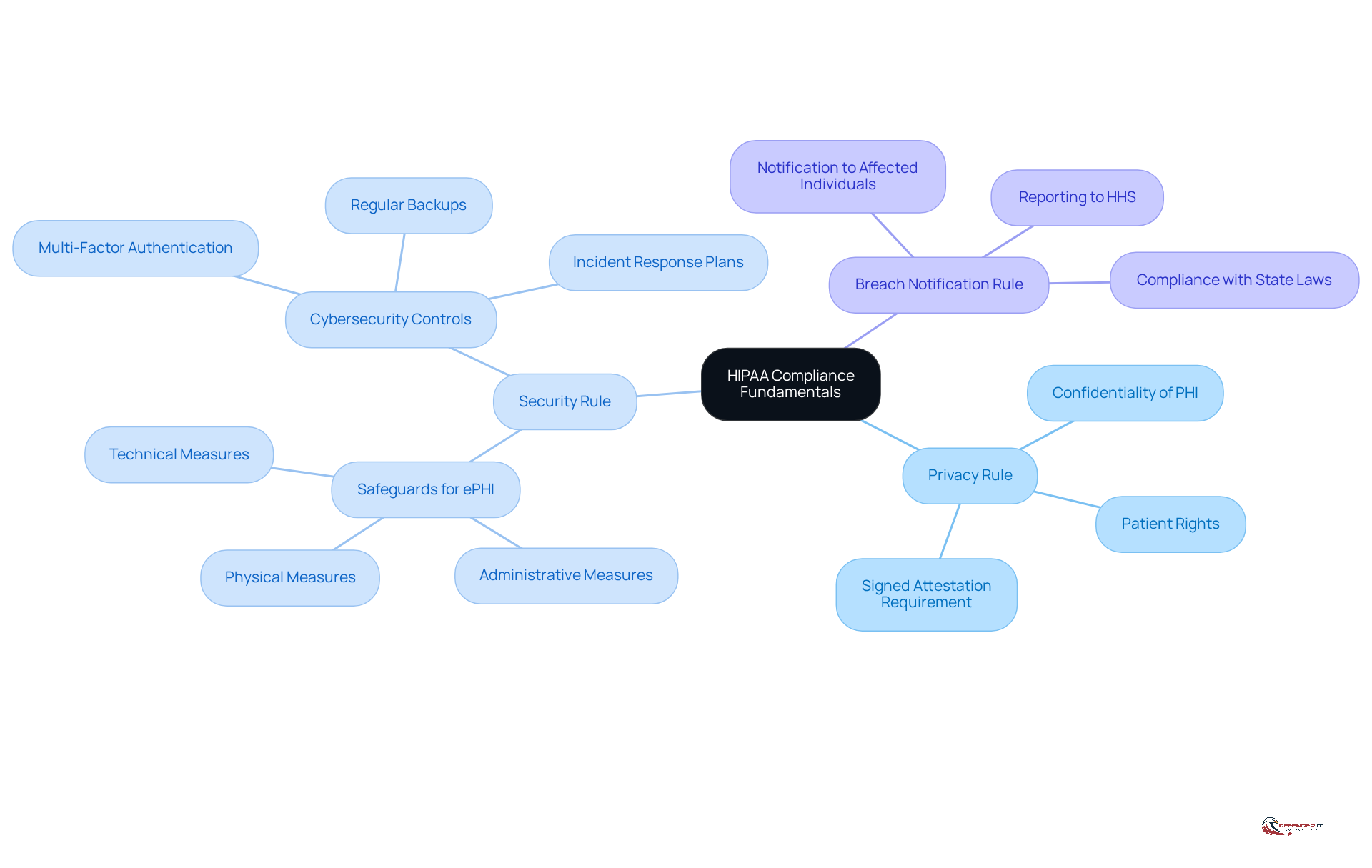
HIPAA, or the Health Insurance Portability and Accountability Act, establishes national standards for the protection of health information. Understanding its is essential for any entity handling protected health information (PHI) in the context of a [HIPAA consultation](https://defenderit.consulting). The main elements include:
- Privacy Rule: This rule establishes standards for the protection of PHI, ensuring that patient information remains confidential.
- Security Rule: It outlines the necessary safeguards to protect electronic PHI (ePHI), which include administrative, physical, and technical measures.
- Breach Notification Rule: This rule requires covered entities to notify affected individuals and the Department of Health and Human Services (HHS) in the event of a data breach.
By grasping these fundamentals, companies can enhance their [compliance readiness](https://defenderit.consulting/4-best-practices-for-effective-nt-hash-implementation-in-cybersecurity/) and mitigate risks associated with non-adherence through HIPAA consultation.
Implement Comprehensive Compliance Programs
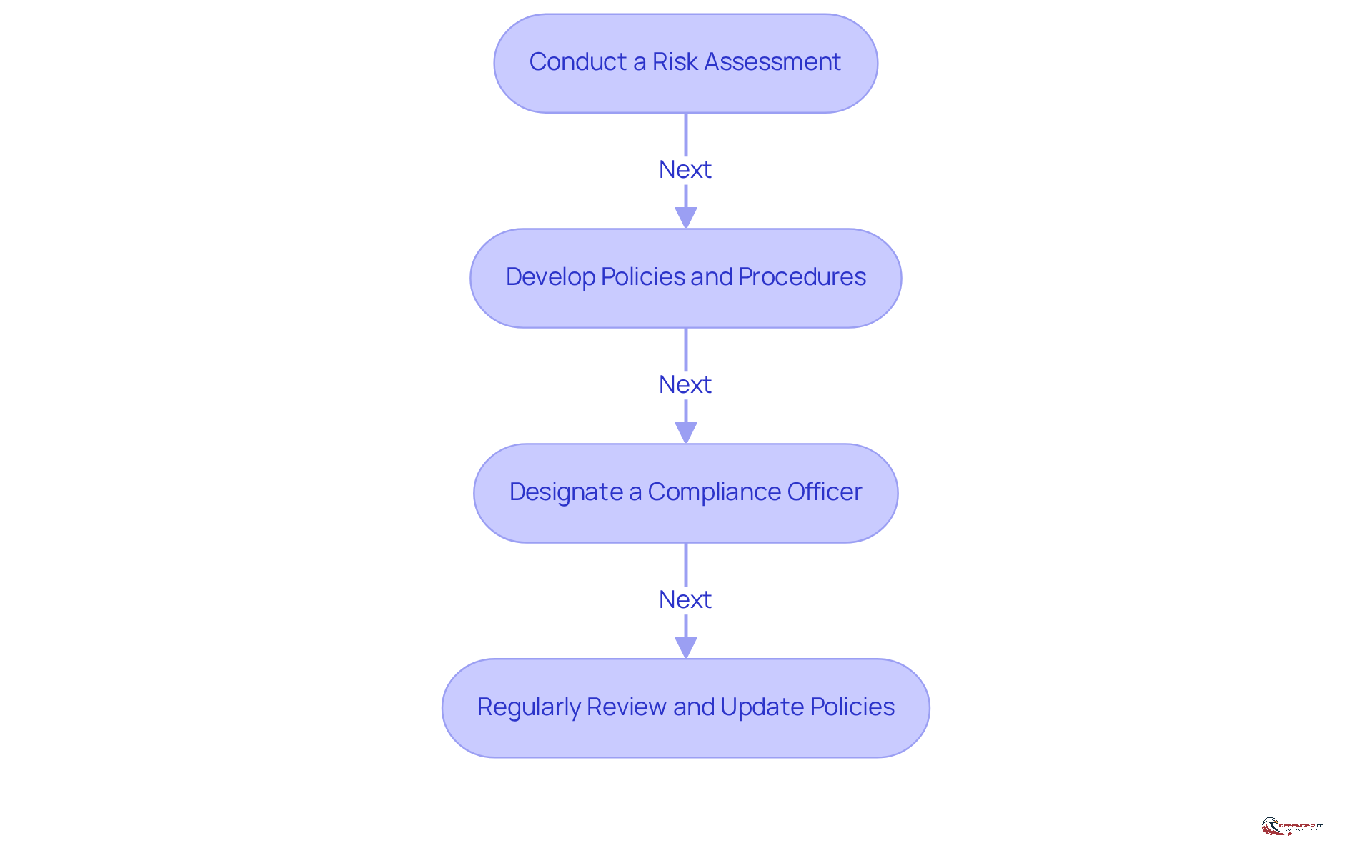
To establish a comprehensive HIPAA compliance program, organizations should prioritize the following steps:
- Conduct a Risk Assessment: Regular risk assessments are essential for identifying vulnerabilities in systems and processes that could lead to breaches of Protected Health Information (PHI). Approximately 70% of healthcare organizations have reported having written privacy policies; however, many still struggle with effective implementation of risk assessments. The maximum penalty for HIPAA violations is currently set at $1.5 million per violation category, per year, underscoring the financial implications of non-compliance.
- Developing policies and procedures through HIPAA consultation is crucial for outlining adherence strategies. These documents should reflect the latest regulatory changes, including updates related to reproductive health care privacy, which took effect in 2024. Organizations must also retain regulatory documentation, risk assessments, training logs, and breach records for a minimum of six years to ensure audit preparedness.
- Designate a Compliance Officer: Appointing a dedicated officer for regulatory oversight is vital for ensuring adherence to health information standards. This individual should coordinate all adherence efforts and ensure that staff are trained on the latest requirements. Furthermore, entities should designate a privacy officer and a security officer to effectively supervise adherence to health information regulations.
- Regularly reviewing and updating policies through HIPAA consultation is crucial, as compliance is not a one-time effort; it requires ongoing attention. Regular reviews and updates of policies are necessary to align with evolving regulations and organizational practices. This proactive approach aids in and fosters patient trust.
By applying these measures, entities can establish a robust healthcare regulation framework that reduces risks and enhances the safeguarding of patient data.
Conduct Regular Staff Training and Awareness Programs
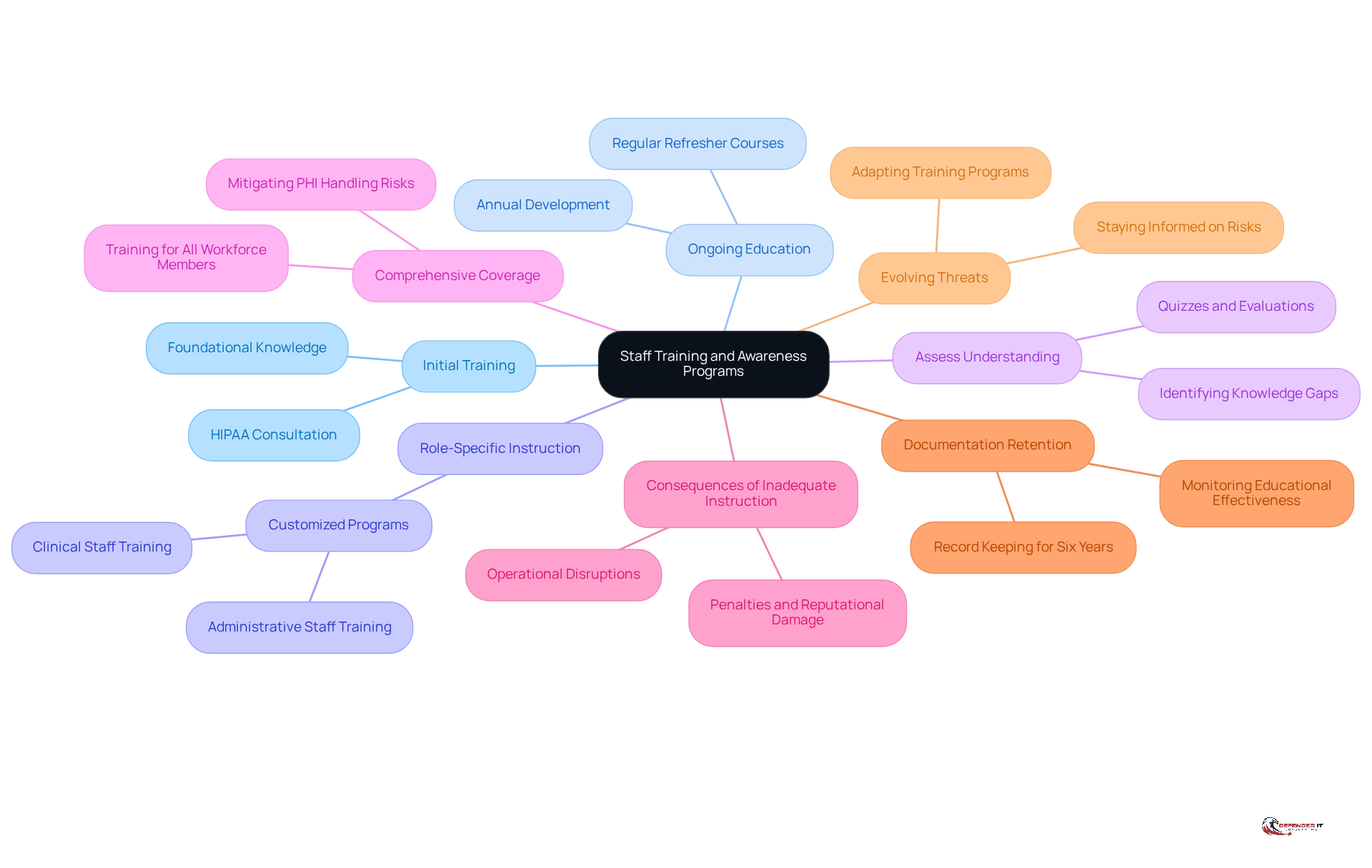
To ensure that all employees are equipped to handle protected health information (PHI) responsibly, organizations must implement effective training strategies that include HIPAA consultation.
Initial training includes a HIPAA consultation to provide comprehensive training for all new employees on HIPAA regulations and organizational policies regarding PHI. This foundational knowledge sets the stage for compliance and awareness.
Ongoing education should include HIPAA consultation, with regular refresher courses scheduled to keep staff updated on changes in HIPAA regulations and best practices. Annual development is regarded as a best practice in the healthcare sector, emphasizing the significance of ongoing learning.
- Role-Specific Instruction: Customizing educational programs to meet the particular duties of various positions within the organization increases relevance and engagement. For instance, clinical staff may require different instruction than administrative personnel, ensuring that all employees understand their unique compliance responsibilities.
- Assess Understanding: Utilizing quizzes or evaluations to gauge employee comprehension and retention of health information privacy materials is crucial. This approach not only reinforces learning but also identifies areas where further education may be needed.
- Comprehensive Coverage: It is vital to ensure that all workforce members, including non-employed individuals, receive HIPAA education to mitigate risks associated with PHI handling. This broad approach helps create a culture of compliance across the organization.
Consequences of inadequate instruction: Organizations must recognize that failing to provide effective education can lead to significant penalties and reputational damage, highlighting the importance of a HIPAA consultation. Understanding these risks underscores the .
- Documentation Retention: Organizations should maintain records of HIPAA instruction for a minimum of six years to comply with documentation requirements. This practice not only promotes adherence but also assists in monitoring educational effectiveness.
- Evolving Threats: Given the continuously changing nature of threats to patient data, ongoing education and adaptation in development programs are essential. This guarantees that staff remain alert and knowledgeable about the latest risks and regulatory requirements.
By prioritizing these training strategies, companies can cultivate a knowledgeable and vigilant workforce, significantly enhancing their adherence to regulations.
Establish Continuous Monitoring and Auditing Processes
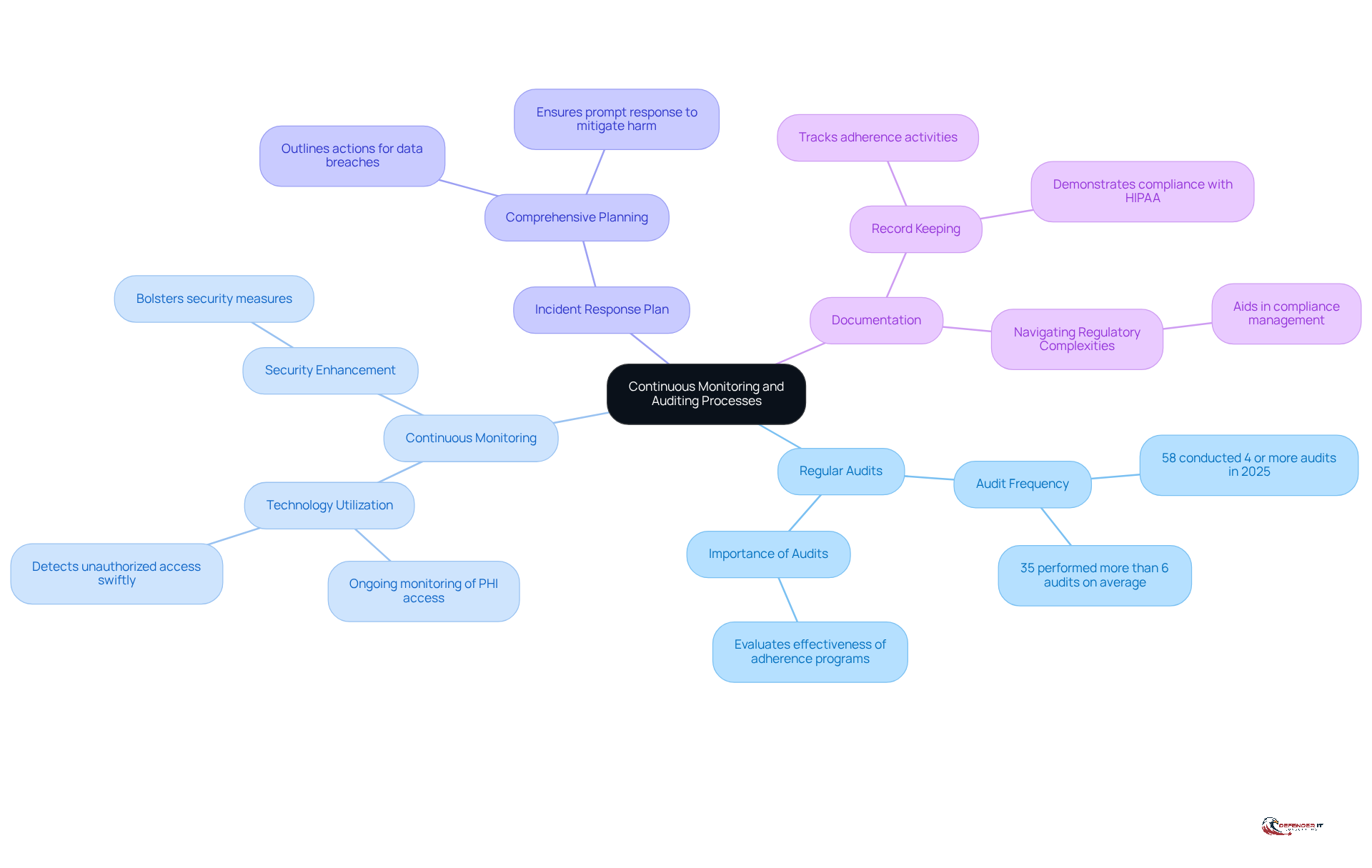
To ensure , entities must implement robust monitoring and auditing practices that safeguard patient information. The following key strategies are essential:
- Regular Audits: Periodic audits are crucial for evaluating the effectiveness of adherence programs. Notably, 58% of entities conducted four or more audits in 2025, with 35% performing more than six audits on average. This trend underscores the increasing focus on compliance oversight.
- Continuous Monitoring: Utilizing technology for ongoing monitoring of access to Protected Health Information (PHI) is vital. This strategy enables entities to swiftly detect unauthorized access and anomalies in data handling, thereby bolstering security measures.
- Incident Response Plan: Crafting a comprehensive incident response plan is imperative. This plan should outline the necessary actions to take in the event of a data breach, ensuring that entities can respond promptly to mitigate potential harm and fulfill regulatory obligations.
- Documentation: Keeping detailed records of all adherence activities-including training sessions, audits, and incident responses-is essential. This documentation not only demonstrates compliance with HIPAA regulations but also aids entities in navigating regulatory complexities.
By implementing these strategies and seeking [HIPAA consultation](https://defenderit.consulting), entities can proactively manage adherence and effectively protect patient data, thereby reducing the risk of costly breaches associated with noncompliance, which averaged $4.61 million in 2025. Furthermore, breaches linked to noncompliance incurred an average additional cost of $174,000, highlighting the financial implications of insufficient compliance practices.
Conclusion
The significance of effective HIPAA consultation practices cannot be overstated for healthcare organizations committed to protecting patient data and ensuring compliance. By concentrating on the fundamental components of HIPAA-namely, the Privacy Rule, Security Rule, and Breach Notification Rule-organizations can lay a robust foundation for safeguarding protected health information (PHI). This foundational understanding is vital for fostering a culture of compliance that permeates every level of the organization.
This article delineates several best practices essential for achieving effective HIPAA consultation:
- Conducting thorough risk assessments
- Developing comprehensive compliance programs
- Providing ongoing staff training
- Establishing continuous monitoring and auditing processes
Each of these practices is crucial in ensuring that organizations not only adhere to current regulations but also adapt to the ever-evolving landscape of healthcare privacy and security. By prioritizing these strategies, organizations can significantly mitigate their risk of breaches and enhance their capacity to respond effectively to potential incidents.
Ultimately, HIPAA compliance represents more than just a regulatory obligation; it embodies a commitment to safeguarding patient rights and nurturing trust within the healthcare system. Organizations must take proactive measures to implement these best practices and continuously refine their compliance efforts. By doing so, they not only protect their operations from costly penalties but also contribute to a more secure and trustworthy healthcare environment that prioritizes patient privacy.
Frequently Asked Questions
What is HIPAA?
HIPAA, or the Health Insurance Portability and Accountability Act, establishes national standards for the protection of health information.
What are the main components of HIPAA compliance?
The main components of HIPAA compliance include the Privacy Rule, Security Rule, and Breach Notification Rule.
What does the Privacy Rule entail?
The Privacy Rule establishes standards for the protection of protected health information (PHI), ensuring that patient information remains confidential.
What is the Security Rule?
The Security Rule outlines the necessary safeguards to protect electronic protected health information (ePHI), which includes administrative, physical, and technical measures.
What is the Breach Notification Rule?
The Breach Notification Rule requires covered entities to notify affected individuals and the Department of Health and Human Services (HHS) in the event of a data breach.
How can understanding HIPAA fundamentals benefit companies?
By grasping these fundamentals, companies can enhance their compliance readiness and mitigate risks associated with non-adherence through HIPAA consultation.